There is now widespread agreement that global warming is occurring and that it is likely to destabilize climatic conditions around the world. Changes in climate will, in turn, result in changes in the environmental determinants of health as well as in the frequency of extreme environmental conditions such as heat waves, floods and droughts. A warmer climate could also mean higher levels of some air pollutants and increased transmission of disease through unclean water and contaminated food. This process would have drastic effects on human health worldwide, including that of Europeans.
Indeed, the 2003 heat wave overwhelmed unprepared healthcare services. WHO attributes over 70,000 deaths in Europe to the 2003 heat wave. Studies now estimate that the extreme temperatures reached in 2003 will be the norm in Europe by the second half of this century. At the same time, global warming could halt the flow of the Gulf Stream system, bringing severe winters to northern, central and eastern Europe.
The relationships between climate change, determinants and health are complex. In addition to the direct impact of changing environmental conditions on human health, health systems, social and economic relationships, and livelihoods will also be affected. Disease caused, transmitted or harboured by insects, snails and other cold-blooded animals can be affected by a changing climate. Organisms such as these, which act as intermediate hosts between pathogens and humans, are disease vectors. The best-known examples are malarial mosquitoes. Climate change could allow such disease vectors to spread to areas where they have not previously been able to survive. While some concern has been raised over the potential spread of malaria to southern Europe, a more probable health threat in Europe is likely to come from changes in the geographic distribution of diseases such as Lyme disease and tick-borne encephalitis, and to increased rates of salmonella and other food-borne infections. Climate change policies must simultaneously address aspects of both climate change mitigation and adaptation.
The 6th Environment and Health Action Programme includes consideration of the need to adapt the European health and emergency infrastructure to address such issues; these policies are being further elaborated in a white paper on climate change adaptation (due between January and February 2009). According to WHO’s contribution to a joint UN consultation for the white paper, the “strengthening of public health systems is already necessary; climate change makes this need even more critical. Besides the possibility of forced migrants due to climatic reasons in and to Europe, there is the much larger health impact outside Europe. Children would be a particularly vulnerable group. EU policies should consider the health implications for its population and those of developing countries. Effective disease surveillance and control become even more important under conditions of rapid environmental change and movement of people, disease vectors and infections. Rapid and accurate disease notification, in compliance with the International Health Regulations, is the essential basis for planning disease control. Approaches such as integrated vector management make the best use of proven interventions to control diseases that may otherwise expand through climate change. For the EU’s own health security it is essential that the strengthening of public health systems in developing countries be addressed in EU foreign policy in the context of climate change adaptation and mitigation.”
More on European Climate Change Policy and Health
Further Definitions
The Relationships between Climate Change, Determinants and Health:
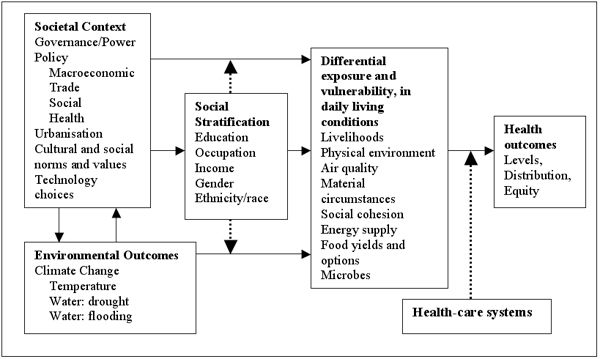
Mitigation:
The EU’s goal is to limit global warming to less than 2°C above the pre-industrial temperature as there is strong scientific evidence that climate change will become dangerous beyond this point. The EU strives to take the lead internationally to ensure this. On January 28th 2009 the EU published its proposals for a global pact on climate change to be negotiated at the Copenhagen climate change conference in December 2009. To stay below 2°C, global emissions need to peak before 2020 and then be cut to less than 50% of 1990 levels by 2050. The EU had already established policies to unilaterally reduce green house gas emissions by 20%; however, limiting global warming to 2 degrees requires that developed countries reduce emissions by 30% by 2020 accompanied by limitations in growth in developing countries of between 15-30%. Estimates suggest that to accomplish this, global net investments will need to rise to EUR 175 billion by 2020, with more than half of this invested in developing countries. To achieve this, the EU calls for an exploration of new innovative sources of funding including an OECD-wide carbon market to be established by 2015 by linking the EU ETS (the EU carbon trading scheme) with other comparable cap-and-trade systems. The market should be expanded to include major emerging economies by 2020 with a view to building a global carbon market. After the difficulties of establishing reforms under the Kyoto Protocol, it is essential that a global agreement be reached in Copenhagen.
Adaptation:
Policies will be a major component of any global pact on climate change. The European Commission’s 2007 green paper on climate change adaptation, gives adaptation the following definition: “Adaptation actions are taken to cope with a changing climate, e.g. increased rainfall, higher temperatures, scarcer water resources or more frequent storms, [either] at present or anticipating such changes in future. Adaptation aims at reducing the risk and damage from current and future harmful impacts cost-effectively or exploiting potential benefits […] Adaptation can encompass national or regional strategies as well as practical steps taken at community level or by individuals. Adaptation measures can be anticipatory or reactive. Adaptation applies to natural as well as to human systems.”
Strengthening health systems in Europe and around the world must be an integral aspect of any adaptation policy. According to a WHO report, currently each year about 800,000 people die worldwide from causes attributable to urban air pollution, 1.8 million from diarrhoea largely resulting from lack of access to clean water supply and sanitation, and from poor hygiene, 3.5 million from malnutrition and approximately 60,000 in natural disasters. This is estimated only to worsen under the effects of global warming. The WHO already attributes 150,000 deaths and 5 million cases of illness to climate change and suggests this will double over the next 25 years.
